The five-year survival of Chinese cancer patients is significantly lower than that of American patients. However, in the past ten years, its survival has increased by 10%. There are many factors for this increased survival, and Chinese medicine played an important role.
Advantages of Chinese medicine on tumors:
1. Emphasize the concept of people-oriented therapy and living with tumors peacefully.
This is a theoretical innovation.
Let’s first look at two examples of gastric cancer.
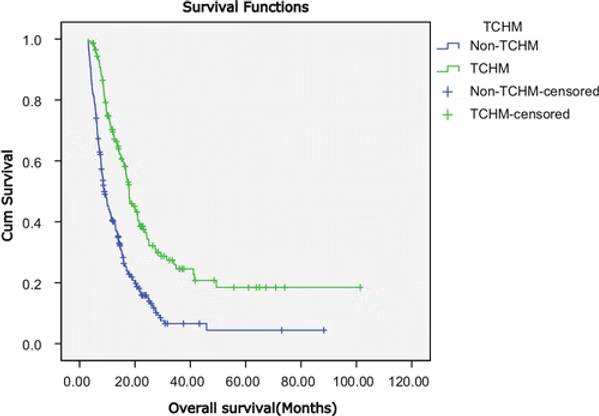
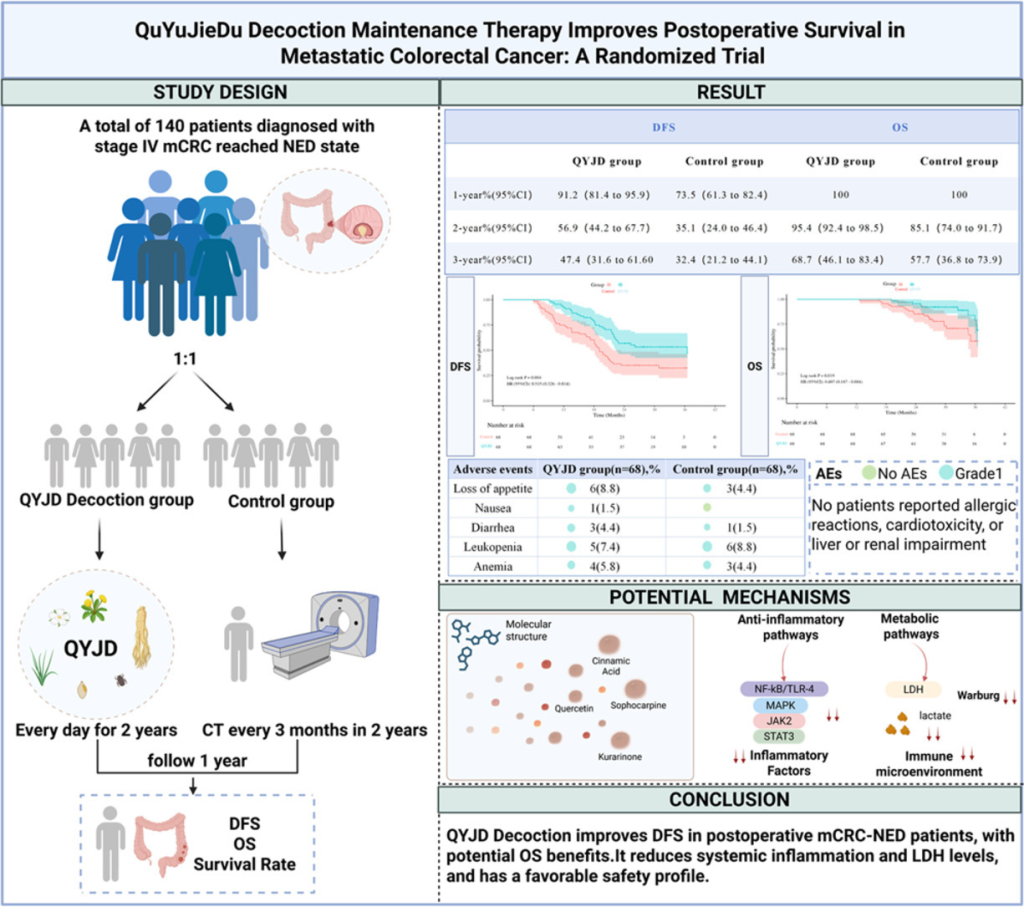
In the figure above, the median survival of patients taking traditional Chinese medicine was 17.9 months, while the median survival of patients not taking traditional Chinese medicine is 8.9 months. That means the life expectancy of patients taking traditional Chinese medicine is twice as long as those not taking it.
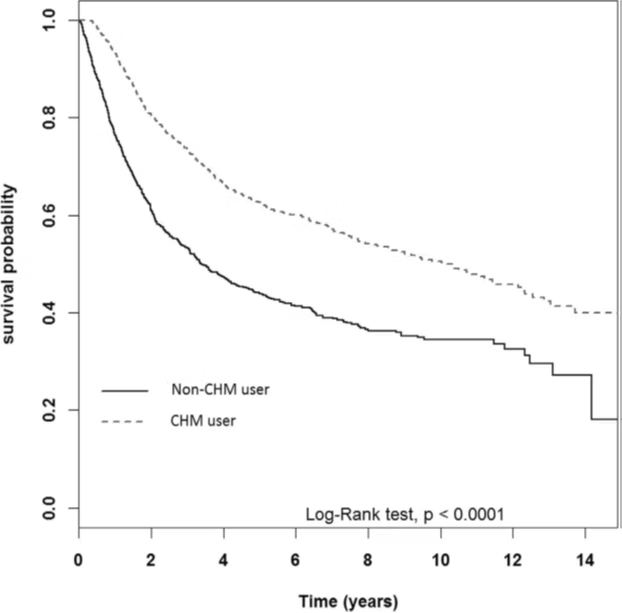
Figure 2 represents the experience of the entire Taiwan region. Similarly, patients who took
traditional Chinese medicine have significantly longer survival than those who did not. They also analyzed the 14-year survival rate of gastric cancer patients and found that it was 40% in the patients who used Chinese medicines, while only 18% in those who did not take Chinese medicines. Again, the use of Chinese medicines prolonged survival by more than twice. Further analysis found that even for patients taking traditional Chinese medicine, the adjusted hazard ratio (aHR) of taking Chinese medicine for more than 180 days a year is 0.37, while for patients taking 30-100 doses a year, it is 0.92. In other words, the survival of the former group is more than twice as long as that of the latter. Roughly speaking, patients who take traditional Chinese medicine for more than 180 days a year will survive at least four times longer than those who do not take traditional Chinese medicine. This once again illustrates the importance of the long-term use of Chinese medicine.
According to our experience, surgical treatment of solid tumors is currently the only promising method to cure tumors (no tumors in five years). Other therapies such as chemotherapy and immunotherapy, if they have little effect on tumor shrinkage after standard courses, or produce strong side effects, continuing this type of treatment will significantly reduce the quality of life and shorten the patient’s survival. On the contrary, adding Chinese medicine treatment can significantly prolong life, improve quality of life, and prevent tumor metastasis and recurrence. In other words, after decades of efforts in the Chinese medicine community, a new tumor treatment concept has emerged: it should focus on prolonging the life expectancy of patients and improving the quality of life, instead of only seeking tumor-free or tumor reduction.
2. Increase the effect of radiotherapy and chemotherapy and reduce side effects
Radiotherapy and chemotherapy are important methods of modern medicine for the treatment of malignant tumors. However, although they can directly kill tumor cells, they can also damage normal tissue cells. The side effects of chemotherapy drugs are mainly bone marrow suppression, gastrointestinal adverse reactions, and dysfunction of the heart, liver, and kidneys. Based on syndrome differentiation and treatment, TCM formulates corresponding treatment rules according to the patient’s deficiency of righteous qi (qi, blood, yin, and yang) and the rise and fall of evil qi (phlegm, blood stasis, poison), which can not only improve the efficacy of radiotherapy and chemotherapy but also reduce various side effects in different degrees.
3. Postoperative tune up therapy to promote body recovery
After surgery, malignant tumors often require radiotherapy, chemotherapy, and other treatments to prevent metastasis and recurrence. However, these methods will inevitably produce some side effects, such as nausea and vomiting, inability to eat well, and other gastrointestinal symptoms, as well as decreased white blood cells, etc., which lead to a decline in the patient’s health. Traditional Chinese medicine treatment can effectively alleviate gastrointestinal reactions caused by the above treatments, maintain a normal appetite, facilitate nutrient absorption, and gradually restore physical strength to ensure the smooth completion of radiotherapy and chemotherapy.
4. Prevent metastasis and recurrence
After the phase of surgery, radiotherapy, and chemotherapy, there is still much room for health. Traditional Chinese medicine therapy can further improve the body’s immune function and eliminate carcinogenic internal environmental abnormalities in the body. Induce the differentiation and apoptosis of residual cancer cells, improve the function of various, effectively prevent recurrence and metastasis, and achieve a complete recovery. It fully embodies the concept of “preventive treatment” of Chinese medicine.
According to incomplete statistics, currently, about 70% of cancer patients in China are receiving different levels of traditional Chinese medicine treatment. TCM treatment of tumors has its inherent characteristics and advantages, and it is an indispensable part of the integrative treatment of tumors.
In recent years, the mechanism studies of traditional Chinese medicine on its anti-tumor effects have advanced from the original cellular level to the molecular level and gene level. Studies have shown that: Chinese medicine can attenuate tumors by multiple approaches: inducing cell differentiation, promoting cell apoptosis, regulating immune function, directly killing tumor cells, inhibiting tumor angiogenesis, reversing tumor cell multidrug resistance, anti-mutation effect, and anti-tumor cell metastasis, etc.
In brief, traditional Chinese medicine played an important role in the integrative therapy of tumors and will continue to improve its clinical effectiveness.